BestProductsForMen.org participates in affiliate programs, which means we may earn a commission if you click on a link and make a purchase. This comes at no additional cost to you. We only recommend products we personally trust, use, or believe will provide value to our readers.
Our goal is to provide honest, helpful reviews and recommendations so you can make informed decisions.
Seasonal Affective Disorder in Introverted Men: Why It Feels Different
- SAD is a subtype of major depressive disorder — not just the “winter blues” — and must follow a recurring seasonal cycle for at least two years to be officially diagnosed.
- Introverted men are especially at risk of missing or dismissing SAD symptoms because withdrawal, low energy, and solitude can feel like personality traits rather than warning signs.
- Light therapy is the first-line treatment for winter SAD, but there are several daily habits and therapy options that can help introverted men manage symptoms without feeling overwhelmed or exposed.
- The line between healthy introvert recharging and SAD-driven withdrawal is thin — and knowing the difference could be one of the most important things you read this winter.
- Geography, circadian rhythm disruption, and reduced sunlight exposure all play a measurable role in who develops SAD and how severely it hits.
Most introverted men don’t realize they have seasonal affective disorder — they just think winter makes them tired.
That quiet assumption is exactly what makes SAD so dangerous for introverted men. The symptoms blend in. The withdrawal feels normal. And because introverted men tend to internalize rather than vocalize, the condition deepens in silence before anyone — including the man himself — notices something is actually wrong. Understanding the intersection of introversion and SAD is a critical first step toward breaking that cycle.
What Seasonal Affective Disorder Actually Is
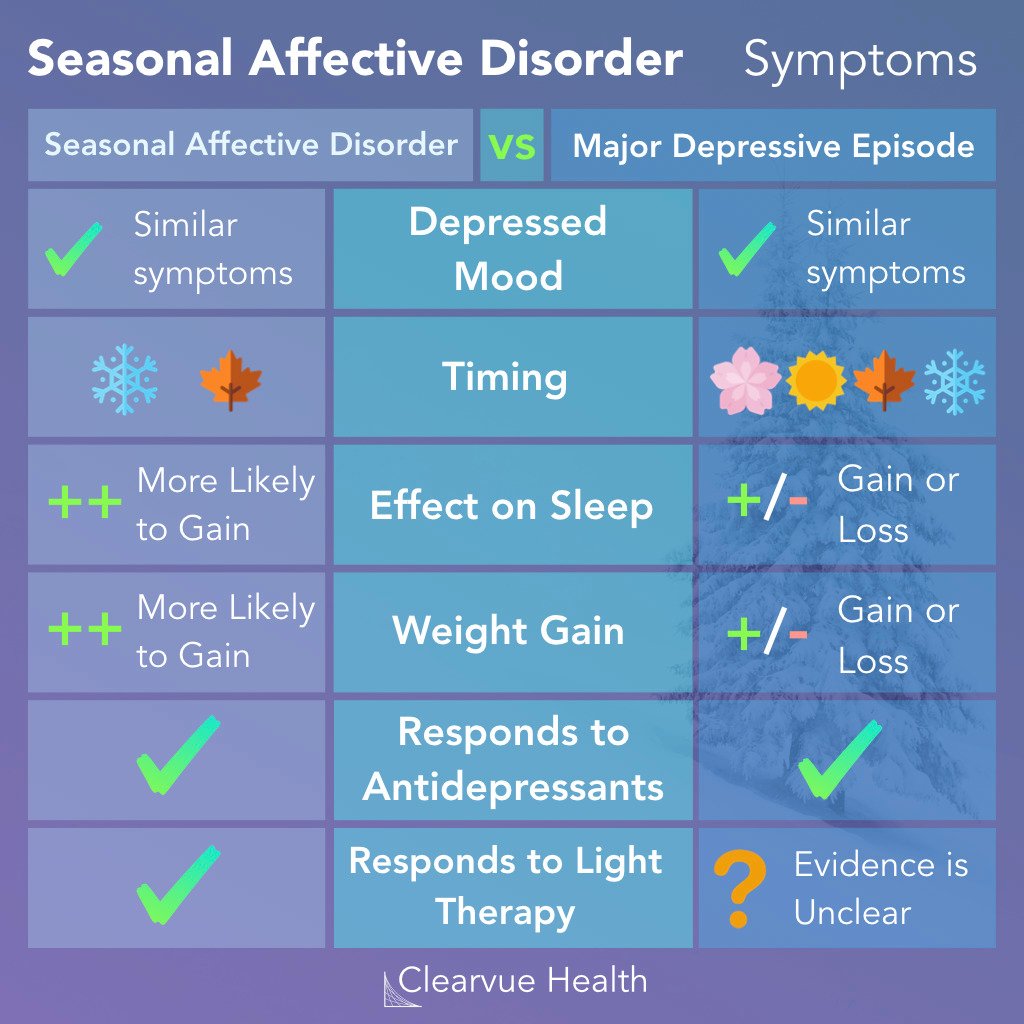
“3 Charts | Seasonal Affective Disorder …” from www.clearvuehealth.com
Seasonal affective disorder is a form of depression that follows a predictable seasonal pattern, most commonly emerging in the fall and winter months when daylight hours shrink and temperatures drop. It’s not a vague mood shift or a case of the “winter blues” — it is a clinically recognized condition with specific diagnostic criteria.
According to Dr. DeSimone, “seasonal affective disorder occurs during certain times of the year, typically in the fall or winter months when there’s less sunlight.” The disorder then resolves as the seasons change, only to return again the following year. That cyclical nature is what separates SAD from generalized depression.
- SAD follows a seasonal pattern tied to reduced sunlight exposure
- It must recur for at least two consecutive years to meet diagnostic criteria
- It is classified as a subtype of major depressive disorder, not a separate condition
- Symptoms go well beyond mood — affecting sleep, appetite, energy, and cognition
- Both winter-onset and summer-onset variations exist, though winter is far more common
SAD Is a Subtype of Major Depressive Disorder
While the name “seasonal affective disorder” is technically informal, it is — as Dr. Ambrose of the American Medical Association noted — “very appropriately initialized as SAD.” More precisely, it is classified as major depressive disorder with a seasonal pattern. That distinction matters because it means SAD carries the full clinical weight of depression, not a lesser mood condition.
To receive a SAD diagnosis, a person must first meet the criteria for major depressive disorder. That means experiencing five of nine recognized depressive symptoms — including anhedonia (loss of pleasure or interest) — for a minimum of two consecutive weeks. The seasonal pattern must then be documented across at least two years.
Dr. Ambrose (AMA): “To meet the criteria for seasonal affective disorder, you must first meet the criteria for major depressive disorder, which is having five of nine symptoms plus anhedonia — that loss of pleasure — for at least two weeks. For some, incorporating omega-3 fatty acids into their diet can be a beneficial supplement.”
This is not a soft diagnosis. When an introverted man is quietly struggling through November and December, telling himself he’s just an introvert who needs more alone time, there’s a real possibility that what he’s experiencing is a full depressive episode — one that will return next year if left unaddressed.
The Seasonal Pattern That Defines SAD
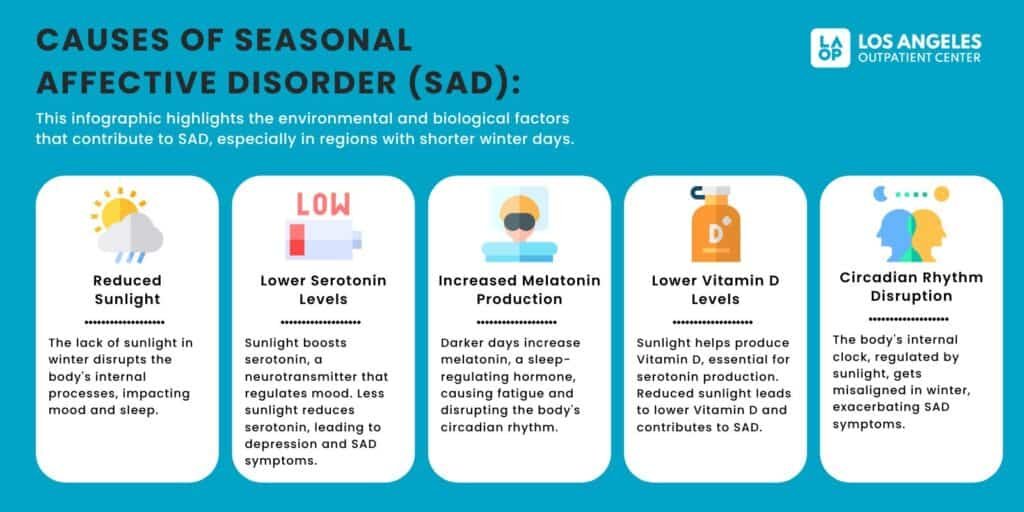
“Seasonal Affective Disorder (SAD …” from laopcenter.com
The leading theory behind SAD connects directly to biology. Reduced sunlight exposure in fall and winter disrupts the body’s circadian rhythm — the internal clock that regulates sleep, hormone production, and mood. This disruption is thought to affect serotonin and melatonin levels in ways that trigger depressive episodes in vulnerable individuals.
Dr. Ambrose (AMA): “Some of the theories behind seasonal affective disorder is it’s linked to the reduced sunlight exposure and circadian rhythm disruption during the winter months.”
One compelling piece of evidence: SAD prevalence increases significantly with geographic latitude. The further you are from the equator, the less winter sunlight you receive — and the higher the reported rates of SAD. This geographic link strongly supports the sunlight-circadian theory and explains why men living in northern climates face a disproportionate risk.
Winter SAD vs. Summer SAD: Two Different Beasts

“Seasonal Depression – CounselingRx” from counselingrx.com
Winter SAD is by far the most common form, characterized by low energy, hypersomnia, carbohydrate cravings, and social withdrawal. Summer SAD, while much rarer, tends to present with the opposite profile — increased anxiety, agitation, insomnia, and restlessness rather than sluggishness. According to Dr. Ambrose, summer SAD produces “more activating symptoms” compared to the vegetative, slowed-down quality of winter SAD. For introverted men, winter SAD is the primary concern — but it’s worth knowing both versions exist.
Why Introverted Men Are Uniquely Vulnerable to SAD
Introversion and SAD share a troubling amount of surface-level overlap. Both involve a preference for solitude, reduced social engagement, lower external stimulation, and a tendency toward internal processing. For an introverted man, the early warning signs of SAD don’t look like alarm bells — they look like Tuesday.
That camouflage is the core problem. When withdrawal feels like a personality trait and low energy feels like a preference, a man can move through an entire SAD episode without ever questioning whether something is clinically wrong. Add to that the cultural conditioning that tells men — especially quiet, self-sufficient men — to handle their problems privately, and you have a setup for chronic underdiagnosis.
How Introversion Amplifies the Urge to Isolate in Winter
Introverted men naturally recharge through solitude. In winter, when the world contracts, the cold sets in, and social invitations dry up, that solitude can feel like relief — at first. But SAD quietly deepens the withdrawal beyond what’s restorative. What starts as healthy alone time can slide into prolonged isolation that reinforces depressive thought patterns, reduces light exposure further, and weakens the social connections that buffer against depression. The introvert doesn’t notice the line being crossed because the behavior looks the same from the outside — and from the inside.
The Mask Men Wear: Why Introverted Men Rarely Speak Up
Men in general are less likely to seek mental health support than women, and introverted men face an additional layer of resistance. They tend to be self-contained, independent thinkers who are uncomfortable processing emotions in social settings. Asking for help — especially for something as invisible as a seasonal mood disorder — can feel foreign or unnecessary. Many introverted men have spent years developing the skill of appearing fine, and that skill works against them when SAD takes hold.
If you’re the kind of man who internalizes stress rather than venting it, that stress doesn’t disappear. It accumulates physiologically. It disrupts sleep. It flattens motivation. Over time, that accumulation looks and feels exactly like depression — because that’s precisely what it is.
The Fine Line Between Introvert Recharging and SAD Withdrawal

“Depressed or introverted? What your …” from introvertspring.com
The single most important distinction for introverted men to understand: healthy introvert recharging feels restorative. You choose solitude, you feel better for it, and you re-engage with the world when you’re ready. SAD-driven withdrawal, by contrast, feels compulsive and joyless. You’re not choosing to be alone because it feels good — you’re avoiding everything because engaging feels impossible. The activities that used to restore you no longer work. That shift in quality — from chosen and restorative to compelled and empty — is the line that separates introversion from a depressive episode.
The Symptoms Introverted Men Miss or Dismiss
SAD doesn’t announce itself. For introverted men, it tends to arrive quietly — layering itself over existing tendencies until the symptoms feel like character rather than condition. Recognizing these specific patterns is what separates early intervention from years of silent suffering. Understanding the role of omega-3 fatty acids in depression management can be a crucial step in this process.
Low Energy That Feels Like Personality, Not Illness
Persistent fatigue is one of the most common SAD symptoms — and one of the easiest for introverted men to rationalize. When you already prefer a slower pace, lower social output, and more time indoors, a significant drop in energy can feel like a natural extension of who you are. But SAD fatigue is qualitatively different. It’s the kind of tired that sleep doesn’t fix, that follows you through the morning no matter how long you stayed in bed, and that makes even low-effort tasks feel disproportionately heavy. If your energy levels drop noticeably every fall and return in spring, that pattern deserves serious attention.
Sleep Disruption and the Hibernate Cycle
Winter SAD frequently produces hypersomnia — sleeping significantly more than usual without feeling rested. For introverted men who already value and protect their sleep and downtime, this can go undetected for weeks. The body’s circadian rhythm is directly disrupted by reduced sunlight exposure, which causes melatonin to be produced at the wrong times and in irregular amounts. The result is a hibernate-like pull: oversleeping on weekends, struggling to get out of bed on weekdays, and feeling perpetually groggy regardless of total sleep hours. This isn’t laziness. It’s a biological response to light deprivation.
Carb Cravings, Weight Gain, and Loss of Motivation
Alongside fatigue and sleep changes, winter SAD commonly triggers intense carbohydrate cravings — particularly for comfort foods high in sugar and starch. This is thought to be connected to the brain’s attempt to regulate serotonin through dietary means, since serotonin production drops when sunlight exposure decreases. For introverted men who may already be prone to solitary eating habits, this craving cycle can accelerate quietly and lead to noticeable weight gain over a winter season.
Motivation collapse is another hallmark symptom that introverted men frequently attribute to preference rather than illness. Projects that were once engaging go untouched. Hobbies that used to provide genuine enjoyment feel hollow or pointless. This is anhedonia — the loss of pleasure in previously rewarding activities — and it is one of the defining criteria for major depressive disorder. When an introverted man stops doing the solo activities he loves, something is clinically wrong.
Common SAD symptoms introverted men often misread as personality traits:
- Low energy — mistaken for introvert preference for a slower pace
- Hypersomnia — mistaken for a love of sleep and downtime
- Social withdrawal — mistaken for healthy recharging
- Loss of motivation — mistaken for laziness or burnout
- Carb cravings — mistaken for comfort-food preference in cold weather
- Anhedonia — mistaken for losing interest in hobbies naturally over time
The pattern across all of these symptoms is the same: they are familiar enough to be dismissed. That familiarity is what makes them so clinically dangerous for introverted men specifically.
When Hopelessness Creeps In Quietly
“Persistent sadness or low moods, and loss of interest or pleasure in activities — since seasonal affective disorder is a subcategory of major depressive disorder, you see a lot of the common symptoms within the two categories.”
— Dr. Ambrose, American Medical AssociationFor those experiencing these symptoms, exploring the role of omega-3 fatty acids in managing depression could be beneficial.
Hopelessness is the symptom that most clearly signals a depressive episode rather than ordinary introvert behavior — and it’s the one men are least likely to name out loud. It doesn’t always feel dramatic. For introverted men, it often presents as a quiet flattening of the future: a sense that things won’t improve, that effort isn’t worth it, that the heaviness is just how life is now. It’s not always dark thoughts. Sometimes it’s just the complete absence of anticipation or possibility.
If that flatness arrives every October and lifts every March, it isn’t your outlook on life. It’s a seasonal depressive pattern — and it’s treatable.
Left unaddressed, these layered symptoms compound. Low energy reduces activity. Reduced activity worsens mood. Isolation deepens. The circadian rhythm destabilizes further. Introverted men who white-knuckle through winter season after season are not building resilience — they’re accumulating damage that gets harder to reverse each year.
How SAD Is Diagnosed
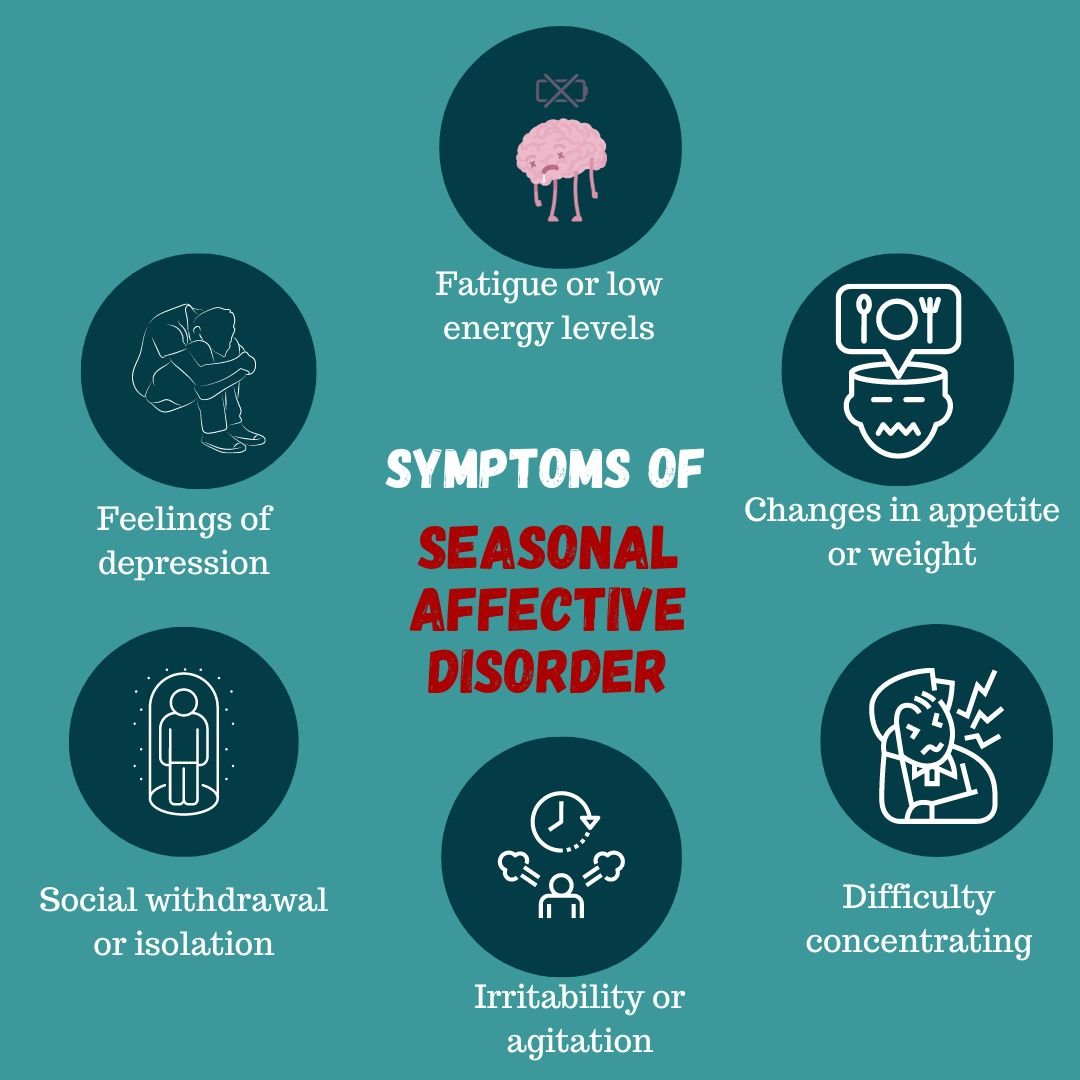
“Seasonal Affective Disorder (SAD …” from continentalhospitals.com
Diagnosis begins with an honest conversation — which is precisely where many introverted men stall. But understanding the actual clinical criteria for SAD removes some of the ambiguity and can make it easier to take that first step. SAD is not diagnosed on the basis of a single bad winter. There is a specific, measurable framework that clinicians use.
The Five of Nine Symptom Criteria for Major Depressive Disorder
Because SAD is classified as major depressive disorder with a seasonal pattern, the diagnostic process starts with MDD criteria. A person must present with at least five of nine recognized symptoms, and those symptoms must include either depressed mood or anhedonia — the two anchor criteria. The nine symptoms are: depressed mood, anhedonia, significant weight change or appetite disturbance, sleep disruption, psychomotor changes, fatigue or loss of energy, feelings of worthlessness or guilt, difficulty concentrating, and recurrent thoughts of death or suicidal ideation.
These symptoms must be present for at least two consecutive weeks and must represent a meaningful change from the person’s baseline functioning. For introverted men, the challenge is recognizing that baseline shift — because several of these symptoms can masquerade as stable personality features rather than clinical departures from normal. Understanding the role of omega-3 fatty acids in depression management can be particularly beneficial in identifying and addressing these changes.
The Two-Year Cycle Requirement for SAD Diagnosis
Beyond the MDD criteria, seasonal affective disorder requires that the depressive episodes follow a consistent seasonal pattern across a minimum of two years — and that full remission also occurs seasonally. According to Dr. DeSimone, “this cycle must occur for two years to meet criteria for the specific type of major depressive disorder.” This two-year threshold is what distinguishes SAD from a single episode of situational depression that happened to occur in winter. If you’ve noticed yourself consistently struggling from October through February for multiple years running, that pattern is clinically significant.
Screening Tools Doctors Use: PHQ-9 and Beyond
The PHQ-9 (Patient Health Questionnaire-9) is the most widely used screening tool for depression in primary care settings. It presents nine questions aligned directly with the MDD diagnostic criteria and produces a scored result that helps clinicians gauge severity. For SAD specifically, some practitioners also use the Seasonal Pattern Assessment Questionnaire (SPAQ) to identify seasonal patterns in mood, sleep, weight, and energy. If you visit a doctor concerned about seasonal mood changes, these are the tools most likely to be used — and knowing that can make the appointment feel less uncertain. Additionally, exploring ashwagandha benefits for stress might offer complementary support for managing seasonal mood variations.
Proven Ways to Manage SAD as an Introverted Man

“Introverted Depression” from www.choosingtherapy.com
The good news: SAD is one of the more treatable forms of depression. The interventions are well-studied, the response rates are strong, and several of the most effective approaches align naturally with the introverted man’s preference for structured, independent, low-stimulation activities.
That last point matters. Many introverted men resist treatment because they imagine it requiring things that feel incompatible with their nature — group therapy, forced socialization, or constant emotional disclosure. In reality, the first-line treatment for winter SAD doesn’t involve any of that, and some men find relief with alternative methods like aromatherapy kits.
Light Therapy: The First-Line Treatment for Winter SAD
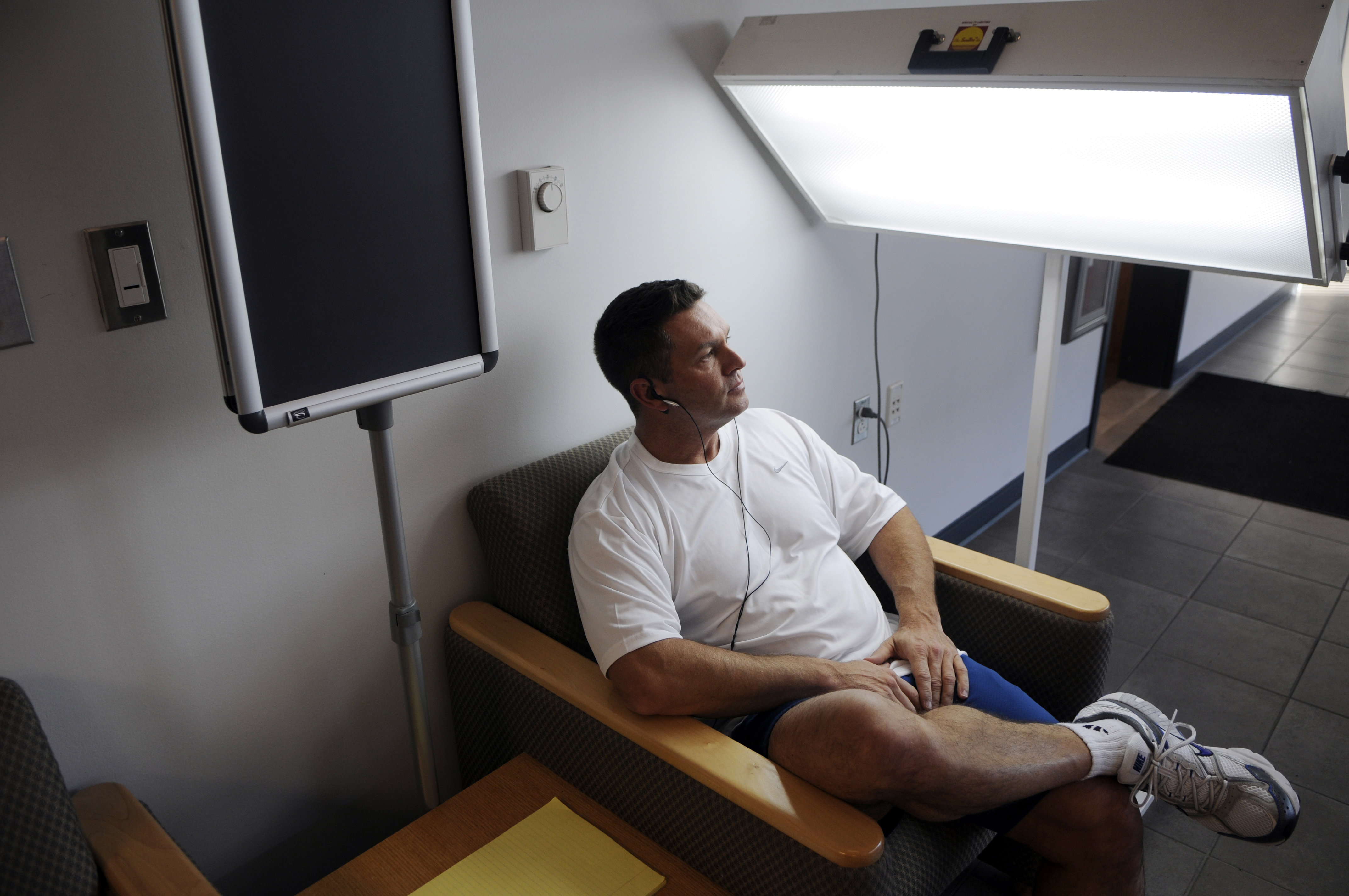
“HAWC shines a light on SADness …” from www.eielson.af.mil and used with no modifications.
Light therapy is the most well-researched, most accessible, and — for many men — most manageable first intervention for winter SAD. It works by exposing the eyes to a bright, full-spectrum light source that mimics natural sunlight, helping to reset the circadian rhythm and suppress the overproduction of melatonin that drives winter depressive symptoms. The effect on mood, energy, and sleep regulation is well-documented, and it doesn’t require talking to anyone, joining anything, or rearranging your social life.
The standard protocol involves a 10,000-lux light therapy lamp used for 20 to 30 minutes each morning, ideally within the first hour of waking. Devices like the Verilux HappyLight Liberty or the Carex Day-Light Classic Plus are purpose-built for this use. Consistency matters more than duration — daily use from early fall through late winter produces significantly better outcomes than sporadic sessions. For an introverted man who already has a structured morning routine, light therapy is a straightforward addition that requires almost nothing socially or emotionally. You sit with your coffee, you run the lamp, you get on with your day, much like incorporating aromatherapy kits for a calming start.
How to Use Therapy Without Feeling Exposed or Overwhelmed
Therapy is one of the most effective treatments for SAD — but the word itself can make introverted men shut down immediately. The image of sitting in a circle sharing feelings, or of being pushed to “open up” before you’re ready, is enough to keep many men from ever making the call. The reality of modern therapy for SAD is considerably more structured and less emotionally invasive than that image suggests.
Cognitive Behavioral Therapy adapted for SAD (CBT-SAD) is the specific modality with the strongest evidence base for this condition. It focuses on identifying and restructuring the negative thought patterns that seasonal depression reinforces — the “this is just how winter is” thinking that keeps introverted men stuck. Sessions are goal-oriented and structured, which tends to suit introverted men far better than open-ended emotional processing formats. To further support mental health, some individuals explore mood tracking apps that can help monitor changes and progress over time.
Teletherapy has also removed one of the biggest practical barriers for introverted men. Platforms like BetterHelp or Talkspace allow you to engage with a licensed therapist from your own space, on your own terms, without waiting rooms or face-to-face pressure. For a man who processes internally and finds social performance exhausting, the ability to type rather than speak — or to sit on his own couch rather than a stranger’s chair — can make the difference between engaging with help and avoiding it entirely.
Daily Habits That Regulate Your Circadian Rhythm
- Wake at the same time every day — including weekends. Circadian rhythm stability depends on consistent anchor points, and irregular sleep timing is one of the fastest ways to worsen seasonal depressive symptoms.
- Get outside within 90 minutes of waking — even on overcast days. Natural light, even diffused through clouds, is significantly more powerful than indoor lighting for circadian signaling.
- Exercise in the morning or early afternoon — physical activity regulates both serotonin and cortisol, and timing it earlier in the day amplifies its circadian benefit without disrupting nighttime sleep.
- Limit blue light exposure after 8 PM — screens suppress melatonin production at exactly the time your body needs it to rise naturally. Blue-light blocking glasses or night mode settings are simple, low-effort solutions.
- Maintain a consistent eating window — the timing of meals sends powerful signals to the body’s secondary circadian clocks. Irregular eating patterns compound the rhythm disruption that SAD already causes.
None of these habits require social energy or emotional vulnerability. They are behavioral and physiological interventions that an introverted man can implement entirely on his own, within his existing routines. That independence is part of what makes them sustainable for this population specifically.
Vitamin D supplementation is also worth discussing with a doctor, particularly for men in northern latitudes. While research on Vitamin D as a standalone SAD treatment is mixed, deficiency is common in winter months and can amplify fatigue and low mood symptoms. A simple blood test can determine whether supplementation is appropriate.
When these habits are stacked together — consistent sleep timing, morning light exposure, regular movement, and reduced evening screen time — the cumulative effect on circadian rhythm stability is meaningful. No single habit is a cure. But the combination creates a physiological environment that is considerably less hospitable to seasonal depression than the default winter lifestyle most introverted men fall into.
When to Get Help and What That Actually Looks Like
The threshold for seeking help is simpler than most introverted men make it. If your mood, energy, motivation, or sleep consistently drops every fall and recovers every spring — and this has happened for more than one year — that pattern warrants a conversation with a doctor. You don’t need to be in crisis. You don’t need to have hit rock bottom. A recurring seasonal pattern that disrupts your functioning is enough.
Start with your primary care physician. Describe the seasonal pattern specifically — when it starts, how long it lasts, what symptoms are most prominent, and how it affects your daily life. Bring up the PHQ-9 if they don’t mention it. Ask whether a referral for CBT-SAD is appropriate. Most primary care doctors are familiar with SAD and can initiate the conversation about light therapy, therapy referrals, or medication options such as bupropion XL, which is the only antidepressant with an FDA-approved indication specifically for the prevention of seasonal depressive episodes.
Getting help as an introverted man doesn’t mean surrendering your independence or your privacy. It means applying the same pragmatic problem-solving approach you use in every other area of your life to a problem that happens to be neurological. You wouldn’t white-knuckle through a broken bone every winter and call it character. SAD deserves the same practical response.
- If symptoms are mild: Start with light therapy, circadian habit adjustments, and daily outdoor exposure — monitor for four to six weeks
- If symptoms are moderate: Add CBT-SAD with a therapist, preferably via teletherapy if in-person feels like a barrier
- If symptoms are severe or include hopelessness: See a doctor promptly — medication combined with therapy has strong evidence for moderate-to-severe SAD
- If you’re having thoughts of self-harm: Contact the 988 Suicide and Crisis Lifeline immediately by calling or texting 988
Frequently Asked Questions
Below are the most common questions introverted men ask about SAD — answered directly, without clinical jargon.
Can introverts mistake SAD for their natural personality?
Yes — and this is one of the most common reasons SAD goes undiagnosed in introverted men. Withdrawal, low social energy, preference for solitude, and reduced enthusiasm can all look like stable introvert traits from the outside. The distinguishing factor is change from your own baseline. If your energy, motivation, and enjoyment of solo activities decline noticeably every fall — regardless of life circumstances — and return every spring, that seasonal shift is not personality. It is a pattern that warrants clinical attention.
Does SAD affect men differently than women?
SAD is diagnosed more frequently in women than men, with some estimates suggesting a 4:1 ratio. However, this disparity likely reflects underreporting rather than true biological immunity in men. Men are significantly less likely to seek mental health treatment, less likely to describe emotional symptoms to a doctor, and more likely to attribute depressive symptoms to external factors like work stress or physical fatigue. For introverted men specifically, the tendency to internalize compounds this underreporting further — meaning male SAD prevalence is almost certainly higher than diagnosis rates suggest. For those looking to manage these symptoms, exploring omega-3 fatty acids for depression could be beneficial.
How long do SAD episodes typically last?
Winter SAD episodes typically begin in late fall — often October or November in the Northern Hemisphere — and resolve naturally in spring, usually by March or April. The average active episode spans four to five months, though this varies by individual and geographic location. During that window, symptoms can fluctuate in intensity, with the darkest months of December and January often representing the peak. For more insights, discover what doctors wish patients knew about Seasonal Affective Disorder.
Without treatment, SAD episodes tend to return each year and can intensify over time. With consistent treatment — particularly the combination of light therapy, behavioral interventions, and therapy — many men experience significantly shorter or less severe episodes. Early intervention in the seasonal cycle, before symptoms fully develop, produces the best outcomes. Starting light therapy in September rather than waiting until symptoms are entrenched in December is a concrete example of how timing shapes results.
Can SAD occur in summer for introverted men?
Summer SAD exists, though it is considerably less common than the winter variety. Where winter SAD produces the low-energy, high-sleep, socially withdrawn presentation that introverted men most often experience, summer SAD tends to manifest with opposite symptoms — increased anxiety, agitation, reduced sleep, and irritability rather than lethargy. For introverted men, who are often already sensitive to overstimulation, the heightened sensory environment of summer — more noise, more social obligation, more disrupted routine — can theoretically contribute to summer-onset depressive episodes. To manage these symptoms, some introverted men find mood tracking apps beneficial for monitoring their emotional well-being.
- Summer SAD symptoms include: insomnia, anxiety, agitation, decreased appetite, and weight loss
- It follows the same two-year cyclical pattern required for a winter SAD diagnosis
- Treatment differs from winter SAD — light restriction rather than light therapy is often involved
- Summer SAD is significantly less researched and less commonly diagnosed than winter SAD
If an introverted man finds that his mood and functioning reliably worsen in summer rather than winter, summer SAD is a legitimate clinical possibility worth raising with a doctor. The seasonal pattern — not the specific season — is the defining diagnostic feature.
It’s also worth noting that some men experience a milder form called subsyndromal SAD, sometimes called the “winter blues,” which doesn’t meet the full diagnostic criteria but still causes meaningful disruption to energy, motivation, and mood. According to Dr. Ambrose, up to one in five U.S. adults experience neurovegetative symptoms of SAD that don’t fully meet criteria — including decreased energy — without qualifying for a full diagnosis. This still warrants attention and can often be managed effectively with the lifestyle interventions described above.
Is SAD more common in certain geographic locations?
Yes — significantly so. The prevalence of SAD increases with distance from the equator, a pattern that directly supports the sunlight-circadian rhythm theory. Men living in northern states like Alaska, Minnesota, or the Pacific Northwest face substantially higher rates of SAD than men in Florida or Texas. The reduced daylight hours in high-latitude winters, combined with frequent overcast skies, create the exact light-deprivation environment that triggers the circadian disruption at the core of SAD.
This geographic pattern also has practical implications for treatment. Men in northern climates may need to begin light therapy earlier in the fall — as early as late August or September — to stay ahead of the seasonal onset. Those in extremely northern latitudes, where winter daylight can drop to just a few hours per day, may require longer daily light therapy sessions or the addition of medication to achieve adequate symptom control. Additionally, incorporating omega-3 fatty acids into their routine could further aid in managing symptoms effectively.
BestProductsForMen.org participates in affiliate programs, which means we may earn a commission if you click on a link and make a purchase. This comes at no additional cost to you. We only recommend products we personally trust, use, or believe will provide value to our readers.
Our goal is to provide honest, helpful reviews and recommendations so you can make informed decisions.


Leave a Reply to Best Paraben-Free Beard Softener for Allergy Season | Seasonal Beard Care Cancel reply