BestProductsForMen.org participates in affiliate programs, which means we may earn a commission if you click on a link and make a purchase. This comes at no additional cost to you. We only recommend products we personally trust, use, or believe will provide value to our readers.
Our goal is to provide honest, helpful reviews and recommendations so you can make informed decisions.
Introduction
Omega-3 for depression has become one of the most researched nutritional strategies in mental health — and for introverted men, it may be especially relevant. Multiple meta-analyses show that omega-3 fatty acids, particularly EPA, can help reduce depressive symptoms, especially in individuals with elevated inflammation.
Introverted men often internalize stress, withdraw socially, and delay seeking support, which can increase vulnerability to low mood. When stress builds quietly over time, inflammation and neurotransmitter imbalance may follow. This is where omega-3 for depression support becomes important — not as a replacement for therapy or medical care, but as a foundational strategy for improving brain health, emotional regulation, and mental clarity.
Understanding how omega-3 fatty acids affect mood, inflammation, and neurotransmitter function can help introverted men take a structured, proactive approach to depression management.
- Omega-3 fatty acids, particularly EPA, have been shown in multiple meta-analyses to reduce depressive symptoms — especially in individuals with high inflammatory markers.
- Introverted men are at a uniquely elevated risk for depression due to stress internalization, social withdrawal patterns, and a cultural reluctance to seek help.
- EPA-dominant omega-3 supplements at doses of 1,000–2,000 mg daily appear to be the most effective formulation for mood support — but the type and dose matter significantly.
- One clinical trial found that 4g of omega-3 daily not only improved depressive symptoms but also enhanced motivation, energy, and alertness in high-inflammation patients.
- Omega-3 is not a replacement for professional mental health care, but it may be one of the most accessible foundational upgrades an introverted man can make for his brain.
Omega-3 and Depression: What Introverted Men Need to Know First
Most men dealing with depression aren’t sitting in a dark room — they’re functioning, showing up, and quietly falling apart on the inside. For introverted men especially, the internal experience of depression is often invisible to everyone around them, including their doctors.
What makes this particularly relevant to omega-3 research is that the biological mechanisms behind depression — inflammation, neurotransmitter disruption, cortisol dysregulation — are the exact systems that omega-3 fatty acids directly influence. Understanding that connection isn’t just interesting science. It’s potentially life-changing information for men who are looking for grounded, evidence-based ways to support their mental health without immediately jumping to pharmaceutical interventions. Resources like Innovative Men’s Health have been exploring this intersection of biology and mental wellness for men who want real answers backed by research.
This isn’t about replacing professional care. It’s about understanding what’s happening in your brain and body — and what you can actually do about it.
Why Introverted Men Face a Higher Depression Risk
Introversion itself isn’t a disorder. But the way introverted men tend to process stress, socialize, and communicate their internal states creates a specific set of depression risk factors that often go unaddressed. For some, exploring ashwagandha benefits for stress can be a helpful tool in managing these challenges.
- Introverted men tend to internalize stress rather than externalizing it through conversation or social connection
- They are more likely to withdraw socially when struggling, which removes natural mood-regulating social contact
- Many carry a strong cultural script around male self-sufficiency that discourages seeking help
- Their depression symptoms often present as low motivation, fatigue, and cognitive fog rather than obvious sadness
- They may go years without a diagnosis because their symptoms don’t match the stereotypical image of depression
Internal Processing and Stress Accumulation
The introvert’s internal world is rich and active — but without an outlet, unprocessed stress becomes a physiological burden. Chronic stress elevates cortisol, which increases inflammatory cytokines, which then disrupt serotonin and dopamine pathways. This is not a metaphor. It is a documented biological cascade that connects emotional suppression to measurable brain chemistry changes.
When stress is repeatedly internalized without release, the hypothalamic-pituitary-adrenal (HPA) axis stays activated for longer periods. This prolonged activation doesn’t just feel bad — it physically degrades the brain’s ability to regulate mood over time. Cortisol literally shrinks the hippocampus, the brain region most associated with emotional regulation and memory.
For introverted men who are high-functioning — holding down jobs, maintaining relationships, appearing fine — this slow accumulation of stress biology is the hidden driver of what eventually surfaces as clinical depression. The body keeps score, even when the man doesn’t.
Social Withdrawal as a Depression Amplifier
“Depression and Social Isolation …” from personalpsychology.com.au
Social connection, even in small doses, is a biological mood regulator — it releases oxytocin, reduces cortisol, and activates reward pathways. When introverted men withdraw during depressive episodes, they inadvertently cut off one of their most effective natural antidepressants. The withdrawal feels protective but functions like fuel on a fire.
The Reluctance to Seek Help
Research consistently shows that men are far less likely than women to seek mental health support, and introverted men face an additional layer of this — the internal experience of depression can feel deeply private, even shameful. Many will exhaust every self-managed option before speaking to anyone, which makes accessible, evidence-based interventions like dietary omega-3 optimization especially important as a first step.
The Omega-3 and Depression Connection
The relationship between omega-3 fatty acids and depression isn’t speculative wellness culture — it’s supported by ecological studies, clinical trials, and comprehensive meta-analyses spanning decades of research. Multiple lines of evidence point in the same direction: low omega-3 status is meaningfully associated with higher rates of depression.
Low Omega-3 Blood Levels Are Common in Depressed Individuals

“Omega-3 Deficiency: Signs and Symptoms” from www.health.com
Clinical studies have demonstrated lower concentrations of omega-3 polyunsaturated fatty acids (PUFAs) in the plasma and red blood cell membranes of depressed individuals compared to non-depressed controls. This isn’t a minor difference — it’s a consistent finding across multiple independent research groups.
Ecological and cross-sectional studies have also reported an inverse association between omega-3 intake and the prevalence of depression across populations. In plain terms: the more omega-3 people consume, the lower the rates of depression in those groups. This association holds across different countries, age groups, and diagnostic criteria.
EPA vs DHA: Which One Matters More for Depression
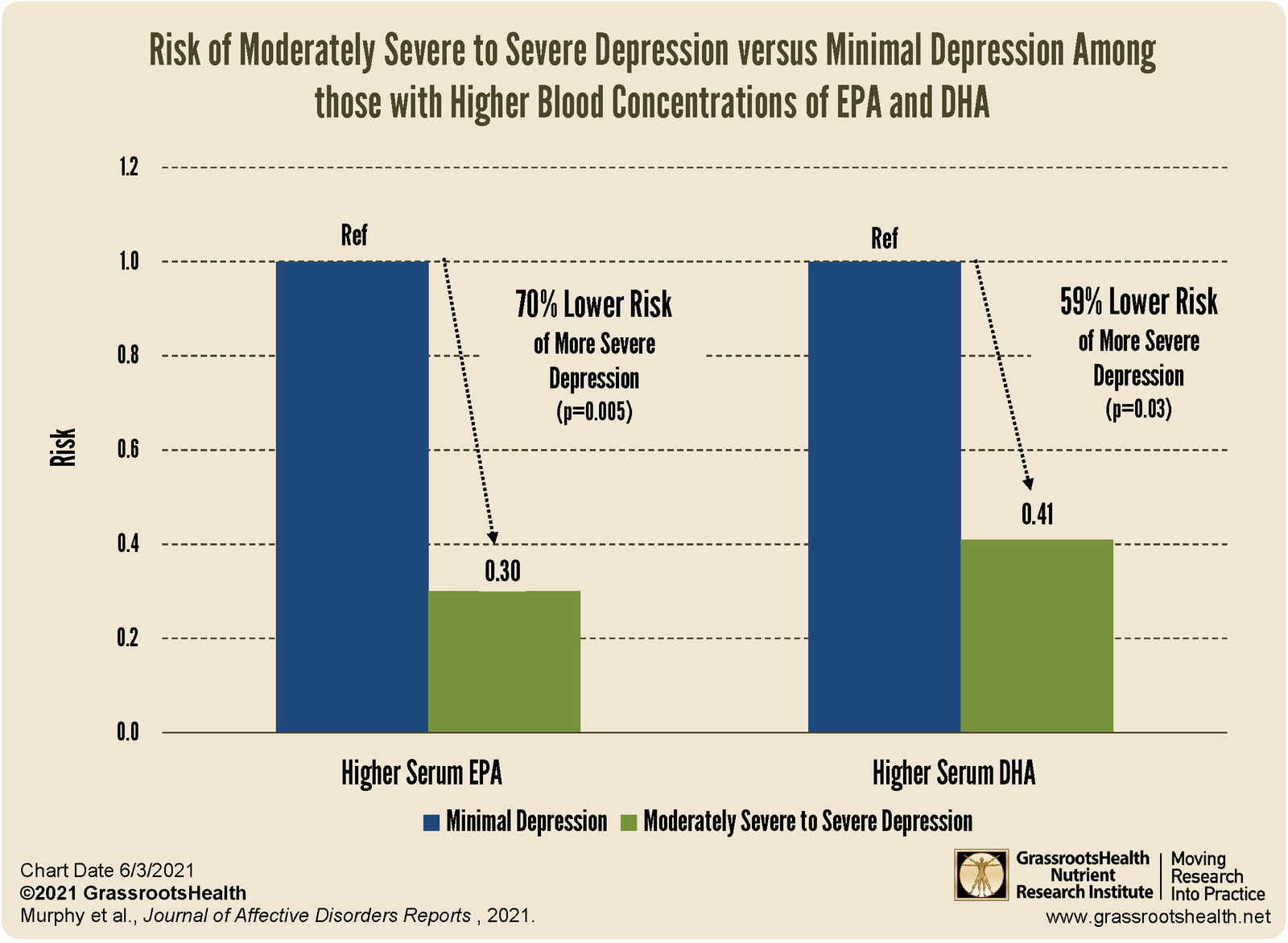
“DHA Related to Lower Depression Scores …” from www.grassrootshealth.net
Both EPA (eicosapentaenoic acid) and DHA (docosahexaenoic acid) are forms of omega-3, but they don’t do the same things in the brain. For depression specifically, EPA appears to be the more therapeutically active compound. Meta-analyses have found that the positive effects of omega-3 supplementation on depressive symptoms depend more heavily on EPA content than DHA content.
Supplements where EPA makes up 60% or more of the total omega-3 content have shown the strongest results in clinical trials focused on depression. DHA is still important for overall brain structure and function, but if you’re targeting mood specifically, EPA-dominant formulas are where the evidence points most clearly.
How Inflammation Links Omega-3 Deficiency to Depression
One of the most compelling explanations for why omega-3s affect mood comes from the inflammation theory of depression. Chronic low-grade inflammation — driven by elevated cytokines like IL-6 and TNF-alpha — disrupts serotonin synthesis, increases cortisol output, and impairs neuroplasticity. Omega-3 fatty acids, particularly EPA, are potent anti-inflammatory agents that directly counteract this process at the cellular level.
Research has specifically found that omega-3 fatty acids may be particularly effective for depression in individuals with elevated inflammatory markers — which is exactly the biological profile that chronic stress and social isolation tend to produce in introverted men who internalize rather than express their emotional states.
How Omega-3 Works in the Depressed Brain
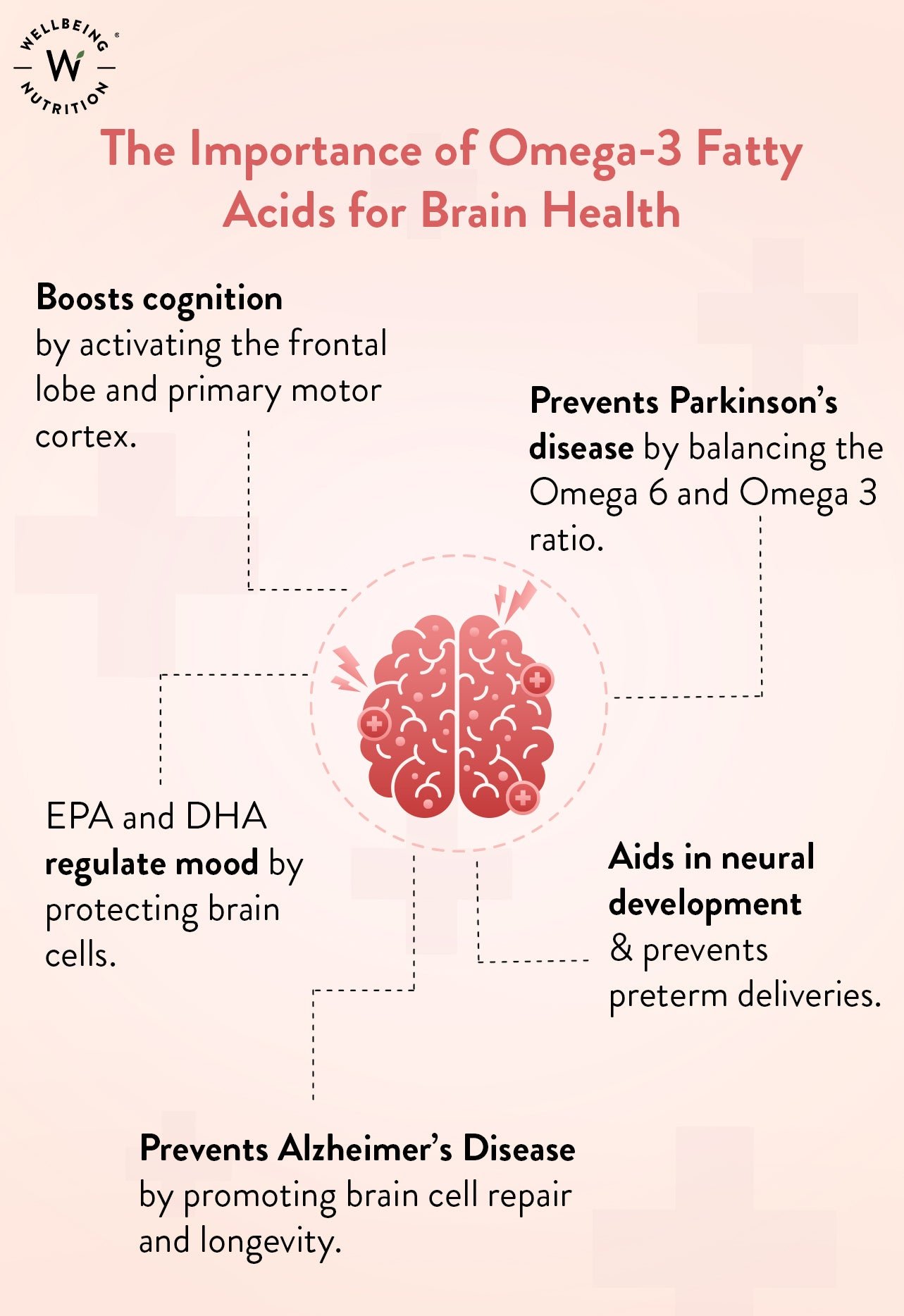
“Omega-3 for Brain & Mental Health” from wellbeingnutrition.com
Understanding the mechanism matters — not just because it’s fascinating biology, but because it explains why omega-3 works for some people and not others, and what conditions make it most effective. The brain is not a fixed organ. It responds to what you put in your body, and omega-3s have several direct pathways through which they influence mood and cognitive function.
Depression at the neurobiological level involves impaired signaling, elevated inflammation, structural degradation of key brain regions, and disrupted neurotransmitter balance. Omega-3 fatty acids interact with all four of these systems — which is why their effects on depression are broader and more fundamental than most people realize.
Omega-3s Reduce Inflammatory Markers Linked to Depression
EPA in particular works as a competitive inhibitor of arachidonic acid, a pro-inflammatory fatty acid. By reducing the production of inflammatory eicosanoids and cytokines, EPA directly lowers the neuroinflammatory environment that impairs serotonin availability and promotes depressive symptoms. This anti-inflammatory action is measurable through blood markers and has been documented in randomized clinical trials.
For men with depression that presents with fatigue, cognitive slowing, and motivational deficits — symptoms strongly associated with inflammatory phenotypes — this mechanism is especially relevant. The inflammation isn’t just a side effect of depression; in many cases, it’s a primary driver of it. To explore ways to manage these symptoms, consider engaging in solo adventure travel experiences which can offer therapeutic benefits.
Cell Membrane Fluidity and Neurotransmitter Signaling
Every neuron in your brain is wrapped in a membrane made largely of fatty acids. The ratio of omega-3 to omega-6 fats in that membrane directly determines how fluid and responsive it is — and membrane fluidity controls how efficiently neurotransmitter receptors function. When omega-3 levels are low, membranes become more rigid, and serotonin and dopamine receptors become less sensitive and less efficient at signal transmission.
This is why omega-3 deficiency doesn’t just cause inflammation — it structurally impairs the brain’s ability to use the neurotransmitters it already produces. You could have adequate serotonin levels but still experience depressive symptoms if the receptors responsible for receiving that signal are embedded in a poorly functioning membrane. Increasing EPA and DHA intake directly improves membrane composition, which improves receptor sensitivity and, consequently, mood regulation. For more information on supplements that can enhance mental well-being, explore the benefits of alpha brain supplements.
Cortisol, Chronic Stress, and Brain Structure Protection
Chronic cortisol elevation — the kind produced by sustained stress internalization in introverted men — physically reduces the volume of the hippocampus and prefrontal cortex, both critical for emotional regulation and cognitive flexibility. Omega-3 fatty acids play a documented role in neurogenesis and neuroplasticity, meaning they support the brain’s ability to grow new neurons and maintain structural integrity under stress. Adequate omega-3 intake doesn’t just buffer the emotional effects of stress; it actively protects the brain regions most vulnerable to cortisol damage.
What the Research Actually Says
The science on omega-3 and depression has moved well beyond preliminary associations. There are now multiple large-scale meta-analyses, randomized controlled trials, and dose-finding studies that give us specific, actionable data on how, when, and for whom omega-3 supplementation is most effective for depression management.
What the research also makes clear is that not all omega-3 interventions are equal. The type of omega-3, the EPA-to-DHA ratio, the dose, the duration, and the inflammatory status of the individual all influence outcomes significantly. Understanding these variables is the difference between supplementing with purpose and just taking a capsule and hoping for the best.
Meta-Analysis Findings: Grosso et al. (2014)
One of the most cited analyses on this topic, published in PLoS ONE by Grosso and colleagues in 2014, conducted a comprehensive meta-analysis of randomized clinical trials examining omega-3 PUFAs in the treatment of depressive disorders. The analysis found a significant positive effect of omega-3 supplementation on depressive symptoms, with results indicating that EPA-dominant formulations consistently outperformed DHA-dominant ones.
Critically, the meta-analysis also found that the more severe the depression, the more likely omega-3 supplementation was to produce measurable reductions in symptoms. This is a meaningful finding for men who have been quietly managing moderate-to-severe depression without intervention — it suggests that the individuals who feel they need help most are also the ones most likely to respond to omega-3 optimization.
Higher Doses Show Stronger Results in High-Inflammation Cases
A randomized dose-finding clinical trial published in the Journal of Clinical Psychiatry (Mischoulon, Dunlop, Kinkead, Schettler et al., 2022) specifically examined omega-3 fatty acids for major depressive disorder in individuals with high inflammatory markers. The trial found that omega-3 supplementation produced meaningful improvements in depressive symptoms in this high-inflammation subgroup — which, as discussed, is a profile commonly seen in men who chronically internalize stress. The antidepressant effects were directly linked to the anti-inflammatory properties of the omega-3 fatty acids used.
4g Per Day and Improvements in Motivation and Cognition
One of the more striking findings in recent clinical research is that daily supplementation with 4g of omega-3 fatty acids not only improved depressive symptoms but also produced measurable improvements in cognition related to motivation — specifically energy and alertness — in depressed individuals with an inflammatory phenotype. This is particularly relevant for introverted men whose depression manifests primarily as low drive, mental fog, and exhaustion rather than overt sadness.
These cognitive and motivational improvements matter because they address the functional impairments that most affect quality of life in working men — the inability to focus, initiate tasks, or feel engaged with things that used to matter. When omega-3 supplementation targets the inflammatory root of these symptoms, the results extend well beyond mood into daily performance and engagement with life.
Best Omega-3 Sources for Daily Use

“Getting Adequate Daily Dose of Omega-3 …” from www.truebasics.com
Getting therapeutic levels of EPA and DHA requires more than the occasional piece of grilled fish. Whether through food or supplementation, consistency and dose matter. Here’s what the most effective sources actually look like in practice.
Fatty Fish: Salmon, Sardines, and Mackerel
Fatty fish remain the gold standard dietary source of EPA and DHA. Wild-caught Atlantic salmon delivers approximately 1,500–2,000 mg of combined EPA and DHA per 3.5 oz (100g) serving, while sardines packed in water provide roughly 1,400 mg per the same serving size. Mackerel is similarly dense, offering around 2,600 mg per 100g — making it one of the most cost-effective whole food sources available. For more on the benefits of these nutrients, check out our article on omega-3 fatty acids for depression.
To reach the 1,000–2,000 mg daily threshold that research associates with mood benefits, two to three servings of fatty fish per week can get you close — but not quite there consistently. For men targeting the higher end of therapeutic dosing (closer to 4g daily), supplementation becomes essentially necessary unless fish consumption is unusually high and consistent.
Fish Oil Supplements vs Algae Oil
Fish oil supplements are the most well-researched delivery method for EPA and DHA, and EPA-dominant formulas — where EPA accounts for at least 60% of total omega-3 content — are the most supported by depression-specific research. Algae oil is a plant-based alternative that provides DHA and, in some formulas, EPA as well. It is a viable option for men who avoid fish products, and the DHA derived from algae is biologically identical to that found in fish. However, most algae oil products are DHA-heavy rather than EPA-heavy, which means they are less directly targeted at depression management based on current evidence.
A Practical Action Plan for Introverted Men Dealing With Depression
Knowing the science is one thing. Applying it in a way that actually fits the life of an introverted man — someone who may be high-functioning on the outside but running on empty internally — requires a structured, low-friction approach that doesn’t demand dramatic lifestyle overhauls all at once.
1. Audit Your Sleep, Sunlight, and Movement First

“Wake Up Tired After 8 Hours of Sleep …” from www.bettersleep.com
Before adding any supplement, the three most powerful free interventions for depression need to be assessed honestly. Sleep deprivation alone elevates inflammatory markers, suppresses testosterone, and impairs serotonin regulation — meaning that if you’re sleeping five to six hours a night and adding omega-3, you are partially supplementing against the damage you’re still causing. The same applies to sunlight exposure, which regulates both vitamin D production and circadian rhythm, and physical movement, which is one of the most robustly supported antidepressant interventions in the entire research literature.
Foundation Habit
Minimum Effective Dose
Depression-Relevant Mechanism
Sleep
7–9 hours per night
Reduces cortisol, restores serotonin synthesis
Sunlight Exposure
15–30 min daily (morning)
Vitamin D production, circadian rhythm regulation
Physical Movement
30 min moderate activity, 3–5x per week
BDNF release, neurogenesis, cortisol reduction
EPA-Dominant Omega-3
1,000–2,000 mg EPA+DHA daily
Anti-inflammatory, membrane fluidity, neurotransmitter support
Once these foundations are honestly accounted for, omega-3 supplementation becomes a meaningful addition rather than a band-aid on a larger problem. The combination of consistent sleep, daily sunlight, regular movement, and EPA-dominant omega-3 intake creates the biological conditions under which the brain can actually begin to regulate mood more effectively.
2. Take an EPA-Focused Omega-3 Supplement for at Least 6 to 8 Weeks
The research is clear that EPA-dominant formulas — where EPA comprises at least 60% of total omega-3 content — produce the most consistent results for depression. A practical starting point is 1,000–2,000 mg of combined EPA and DHA daily, taken with a meal containing dietary fat to maximize absorption. If you fall into the high-inflammation category — characterized by fatigue-dominant depression, poor stress recovery, or a history of chronic illness — the clinical evidence supports doses up to 4g daily under appropriate supervision.
Consistency over time is non-negotiable. Omega-3 fatty acids incorporate into cell membranes gradually, meaning the full therapeutic effect isn’t immediate. Most clinical trials showing significant antidepressant effects ran for a minimum of six to eight weeks, and some showed continued improvement at the twelve-week mark. Starting supplementation and abandoning it after two weeks because you don’t feel dramatically different is one of the most common reasons men dismiss omega-3 as ineffective when the biology simply hadn’t had enough time to work.
Two specific products worth knowing: Nordic Naturals Pro EPA delivers 1,060 mg of EPA per two-capsule serving with a favorable EPA-to-DHA ratio, and Carlson Labs Super Omega-3 provides a well-studied fish oil formulation that has been used in clinical research contexts. When selecting a product, look for third-party testing certification, triglyceride form (more bioavailable than ethyl ester form), and an EPA percentage of at least 60% of total omega-3 content.
3. Test Key Biomarkers: Testosterone, Vitamin D, and Thyroid

“10 Vital Biomarkers …” from plexusdx.com and used with no modifications.
Depression in men rarely has a single cause, and omega-3 deficiency rarely operates in isolation. Low testosterone, vitamin D deficiency, and subclinical hypothyroidism are three of the most commonly missed biological contributors to male depression — and all three are correctable once identified. A basic blood panel covering free and total testosterone, 25-hydroxyvitamin D, TSH, free T3, and free T4 gives you a complete picture of the hormonal environment your brain is operating in. Additionally, incorporating ashwagandha benefits can support stress management, which is crucial for mental health.
Vitamin D is particularly worth flagging in the context of omega-3 because both nutrients work through overlapping anti-inflammatory and neuroprotective pathways. Deficiency in both simultaneously — which is extremely common in men who spend most of their time indoors — creates a compounding biological disadvantage that no single intervention alone can fully overcome. Knowing your numbers means knowing where the actual gaps are.
4. Address Full-Body Inflammation Through Diet and Lifestyle
Omega-3 supplementation is most effective when it isn’t fighting against a diet that actively drives inflammation. Processed seed oils high in omega-6 (like soybean, corn, and sunflower oil), refined carbohydrates, excess sugar, and alcohol all elevate the same inflammatory cytokines that omega-3s work to suppress. Improving the omega-3 to omega-6 ratio in your diet — by reducing processed food intake and increasing fatty fish, olive oil, and whole food sources — amplifies the effect of supplementation significantly.
The practical version of this doesn’t require a complete dietary overhaul. Swapping one processed meal per day for a whole food alternative, cooking with olive oil instead of vegetable oil, and adding two to three servings of fatty fish per week creates a measurable shift in inflammatory load without requiring a dramatic lifestyle change — which matters for introverted men who do better with sustainable incremental adjustments than wholesale transformation.
5. Get Professional Support for Persistent Depression
Omega-3 optimization, lifestyle adjustment, and biomarker correction are powerful tools — but they are not a substitute for professional mental health support when depression is persistent, severe, or impairing daily function. A psychiatrist, integrative medicine physician, or therapist familiar with male depression presentations can work alongside the biological interventions discussed here. Seeking that support is not a sign of failure. For introverted men especially, having one trusted professional in your corner can be the highest-leverage thing you do for your mental health.
Omega-3 Is Not a Cure, But It Is a Foundation
Omega-3 fatty acids won’t resolve the root causes of depression on their own — but they correct a biological deficit that makes everything else harder. When your cell membranes are functioning properly, inflammation is controlled, and your brain has the structural raw materials it needs, every other intervention works better. Therapy lands differently. Sleep restores more completely. Exercise produces stronger neurochemical benefits. Think of adequate EPA and DHA intake not as a treatment, but as creating the neurological conditions under which recovery becomes possible.
Frequently Asked Questions
Men researching omega-3 for depression management tend to ask the same practical questions — not about abstract mechanisms, but about timing, dosing, safety, and what to actually buy. The answers below are grounded in the clinical evidence covered throughout this article.
Before diving in, here’s a quick reference for the most important variables that determine whether omega-3 supplementation will work for depression:
- EPA content: Must be at least 60% of total omega-3 for depression-specific benefits
- Daily dose: 1,000–2,000 mg combined EPA/DHA as a starting point; up to 4g for high-inflammation presentations
- Duration: Minimum 6–8 weeks before assessing full effect
- Form: Triglyceride form is more bioavailable than ethyl ester form
- Timing: Take with a fat-containing meal for optimal absorption
Use these variables as your checklist when evaluating any omega-3 product or protocol for mental health purposes.
How Long Does It Take for Omega-3 to Improve Depression Symptoms?
Most clinical trials showing significant antidepressant effects from omega-3 supplementation ran for a minimum of six to eight weeks, with some studies showing continued improvement at the twelve-week mark. The mechanism explains the timeline — omega-3 fatty acids need to incorporate into cell membranes gradually before their effects on receptor sensitivity and inflammatory signaling become fully measurable.
For men with a higher inflammatory load or more severe baseline depression, the trajectory may be slower initially but the magnitude of improvement tends to be greater over time. The key is consistent daily intake without interruption. Missing doses frequently or cycling on and off supplementation disrupts the membrane incorporation process and significantly blunts the therapeutic effect.
What Is the Best Omega-3 Dosage for Depression in Men?
The research supports a starting dose of 1,000–2,000 mg of combined EPA and DHA per day for general depression management, with EPA comprising at least 60% of that total. For individuals with documented high inflammatory markers or more severe depressive presentations, the clinical trial by Mischoulon and colleagues (2022) demonstrated meaningful improvements at 4g daily — though doses at that level should be used with awareness of potential blood-thinning effects, particularly in men taking other medications.
There is no universal perfect dose because individual inflammatory load, dietary baseline, body composition, and severity of depression all influence response. Starting at 1,000–2,000 mg daily, maintaining that consistently for eight weeks, and then evaluating symptoms objectively is a reasonable and evidence-aligned protocol for most men.
Can Introverted Men Take Omega-3 Alongside Antidepressants?
Omega-3 supplementation has been studied as both a standalone intervention and as an adjunctive therapy alongside antidepressant medication, and the research supports its use in both contexts. Several meta-analyses specifically examined omega-3 as an adjuvant treatment and found additive benefits when combined with standard antidepressants. The most important clinical consideration is that high-dose omega-3 (particularly above 3g daily) can have mild anticoagulant effects, which may interact with blood-thinning medications. Always disclose omega-3 supplementation to your prescribing physician when taking any psychiatric or cardiovascular medication.
Is Fish Oil or Algae Oil Better for Mental Health?
Fish oil is the more research-supported option for depression specifically, primarily because most clinical trials used fish-derived EPA and DHA, and because fish oil products are more easily formulated with the EPA-dominant ratios that depression research favors. Algae oil is a legitimate and bioavailable alternative — the DHA in algae oil is structurally identical to that in fish — but most commercially available algae oil products are DHA-heavy rather than EPA-heavy, making them less optimized for mood-specific outcomes. If you avoid fish products entirely, look for algae oil formulas that specifically provide meaningful EPA content alongside DHA.
Does Omega-3 Help With Anxiety as Well as Depression?
The evidence for omega-3 in anxiety management is promising but somewhat less robust than the depression literature. Some studies have shown reductions in anxiety symptoms with omega-3 supplementation, and the anti-inflammatory and HPA axis-regulating mechanisms that make omega-3 relevant for depression are also theoretically applicable to anxiety — particularly anxiety driven by chronic stress and inflammatory load.
For introverted men, anxiety and depression frequently co-occur and share overlapping biological roots. The same EPA-dominant omega-3 protocol that targets depression-related inflammation will likely provide some degree of benefit for anxiety as well, particularly the kind of low-grade, persistent background anxiety that accompanies chronic stress internalization.
What omega-3 is unlikely to resolve on its own is acute anxiety, panic disorder, or anxiety disorders with significant behavioral avoidance components. Those presentations benefit most from structured therapeutic intervention — but having adequate omega-3 status creates a calmer neurobiological baseline from which that therapeutic work becomes more accessible and effective. For introverted men ready to take their mental health seriously from the ground up, Innovative Men’s Health offers evidence-based guidance built specifically around the biology and challenges that men like you actually face.
Omega-3 fatty acids have been shown to play a significant role in managing depression, especially among introverted men. Research indicates that these essential fats can help improve mood and overall mental health. For a deeper understanding of how omega-3 fatty acids for depression can benefit mental well-being, consider exploring more comprehensive studies and articles on the subject.
BestProductsForMen.org participates in affiliate programs, which means we may earn a commission if you click on a link and make a purchase. This comes at no additional cost to you. We only recommend products we personally trust, use, or believe will provide value to our readers.
Our goal is to provide honest, helpful reviews and recommendations so you can make informed decisions.


Leave a Reply to Best Beard Grooming Kits for Beginners Under $50 (2026 Guide) Cancel reply